436 results
Somatic multicomorbidity and disability in patients with psychiatric disorders in comparison to the general population: a quasi-epidemiological investigation in 54,826 subjects from 40 countries (COMET-G study)
- Konstantinos N. Fountoulakis, Grigorios N. Karakatsoulis, Seri Abraham, Kristina Adorjan, Helal Uddin Ahmed, Renato D. Alarcón, Kiyomi Arai, Sani Salihu Auwal, Michael Berk, Sarah Bjedov, Julio Bobes, Teresa Bobes-Bascaran, Julie Bourgin-Duchesnay, Cristina Ana Bredicean, Laurynas Bukelskis, Akaki Burkadze, Indira Indiana Cabrera Abud, Ruby Castilla-Puentes, Marcelo Cetkovich, Hector Colon-Rivera, Ricardo Corral, Carla Cortez-Vergara, Piirika Crepin, Domenico De Berardis, Sergio Zamora Delgado, David De Lucena, Avinash De Sousa, Ramona Di Stefano, Seetal Dodd, Livia Priyanka Elek, Anna Elissa, Berta Erdelyi-Hamza, Gamze Erzin, Martin J. Etchevers, Peter Falkai, Adriana Farcas, Ilya Fedotov, Viktoriia Filatova, Nikolaos K. Fountoulakis, Iryna Frankova, Francesco Franza, Pedro Frias, Tatiana Galako, Cristian J. Garay, Leticia Garcia-Álvarez, Maria Paz García-Portilla, Xenia Gonda, Tomasz M. Gondek, Daniela Morera González, Hilary Gould, Paolo Grandinetti, Arturo Grau, Violeta Groudeva, Michal Hagin, Takayuki Harada, Tasdik M. Hasan, Nurul Azreen Hashim, Jan Hilbig, Sahadat Hossain, Rossitza Iakimova, Mona Ibrahim, Felicia Iftene, Yulia Ignatenko, Matias Irarrazaval, Zaliha Ismail, Jamila Ismayilova, Asaf Jakobs, Miro Jakovljević, Nenad Jakšić, Afzal Javed, Helin Yilmaz Kafali, Sagar Karia, Olga Kazakova, Doaa Khalifa, Olena Khaustova, Steve Koh, Svetlana Kopishinskaia, Korneliia Kosenko, Sotirios A. Koupidis, Illes Kovacs, Barbara Kulig, Alisha Lalljee, Justine Liewig, Abdul Majid, Evgeniia Malashonkova, Khamelia Malik, Najma Iqbal Malik, Gulay Mammadzada, Bilvesh Mandalia, Donatella Marazziti, Darko Marčinko, Stephanie Martinez, Eimantas Matiekus, Gabriela Mejia, Roha Saeed Memon, Xarah Elenne Meza Martínez, Dalia Mickevičiūtė, Roumen Milev, Muftau Mohammed, Alejandro Molina-López, Petr Morozov, Nuru Suleiman Muhammad, Filip Mustač, Mika S. Naor, Amira Nassieb, Alvydas Navickas, Tarek Okasha, Milena Pandova, Anca-Livia Panfil, Liliya Panteleeva, Ion Papava, Mikaella E. Patsali, Alexey Pavlichenko, Bojana Pejuskovic, Mariana Pinto Da Costa, Mikhail Popkov, Dina Popovic, Nor Jannah Nasution Raduan, Francisca Vargas Ramírez, Elmars Rancans, Salmi Razali, Federico Rebok, Anna Rewekant, Elena Ninoska Reyes Flores, María Teresa Rivera-Encinas, Pilar Saiz, Manuel Sánchez de Carmona, David Saucedo Martínez, Jo Anne Saw, Görkem Saygili, Patricia Schneidereit, Bhumika Shah, Tomohiro Shirasaka, Ketevan Silagadze, Satti Sitanggang, Oleg Skugarevsky, Anna Spikina, Sridevi Sira Mahalingappa, Maria Stoyanova, Anna Szczegielniak, Simona Claudia Tamasan, Giuseppe Tavormina, Maurilio Giuseppe Maria Tavormina, Pavlos N. Theodorakis, Mauricio Tohen, Eva Maria Tsapakis, Dina Tukhvatullina, Irfan Ullah, Ratnaraj Vaidya, Johann M. Vega-Dienstmaier, Jelena Vrublevska, Olivera Vukovic, Olga Vysotska, Natalia Widiasih, Anna Yashikhina, Panagiotis E. Prezerakos, Daria Smirnova
-
- Journal:
- CNS Spectrums / Volume 29 / Issue 2 / April 2024
- Published online by Cambridge University Press:
- 25 January 2024, pp. 126-149
-
- Article
-
- You have access Access
- HTML
- Export citation
-
Background
The prevalence of medical illnesses is high among patients with psychiatric disorders. The current study aimed to investigate multi-comorbidity in patients with psychiatric disorders in comparison to the general population. Secondary aims were to investigate factors associated with metabolic syndrome and treatment appropriateness of mental disorders.
MethodsThe sample included 54,826 subjects (64.73% females; 34.15% males; 1.11% nonbinary gender) from 40 countries (COMET-G study). The analysis was based on the registration of previous history that could serve as a fair approximation for the lifetime prevalence of various medical conditions.
ResultsAbout 24.5% reported a history of somatic and 26.14% of mental disorders. Mental disorders were by far the most prevalent group of medical conditions. Comorbidity of any somatic with any mental disorder was reported by 8.21%. One-third to almost two-thirds of somatic patients were also suffering from a mental disorder depending on the severity and multicomorbidity. Bipolar and psychotic patients and to a lesser extent depressives, manifested an earlier (15–20 years) manifestation of somatic multicomorbidity, severe disability, and probably earlier death. The overwhelming majority of patients with mental disorders were not receiving treatment or were being treated in a way that was not recommended. Antipsychotics and antidepressants were not related to the development of metabolic syndrome.
ConclusionsThe finding that one-third to almost two-thirds of somatic patients also suffered from a mental disorder strongly suggests that psychiatry is the field with the most trans-specialty and interdisciplinary value and application points to the importance of teaching psychiatry and mental health in medical schools and also to the need for more technocratically oriented training of psychiatric residents.
The explorer king: southern report of the king penguin (Aptenodytes patagonicus) in the Antarctic Peninsula
- Marcela M. Libertelli, Jose L. Orgeira, Facundo Alvarez
-
- Journal:
- Antarctic Science , First View
- Published online by Cambridge University Press:
- 16 January 2024, pp. 1-4
-
- Article
- Export citation
-
A juvenile king penguin (Aptenodytes patagonicus) was sighted at San Martín Station, Marguerite Bay, west of the Antarctic Peninsula (68°07'S, 67°08'W) on 3 February 2020. The animal was apparently healthy. It was uninjured, moving freely between the station buildings. It remained in the area until 27 March, when it was last seen. Numerous king penguin records have been reported in recent years, mostly in the South Shetland Islands. Two chicks have even been recorded hatching on these islands, but there is currently no evidence that king penguins have raised a chick to emancipation successfully. Here we present the most southerly known record of king penguins, the only one farther south than the Antarctic Circle. Coupled with observations from other parts of Antarctica, the information presented here supports previous suggestions by other authors of a southwards expansion of this species specifically in the Antarctic Peninsula region. The presence of this species at numerous Antarctic localities suggests that the known distribution of this penguin could change in the near future in response to climate change.
Incidence and risk factors for catheter-associated urinary tract infection in 623 intensive care units throughout 37 Asian, African, Eastern European, Latin American, and Middle Eastern nations: A multinational prospective research of INICC
- Victor Daniel Rosenthal, Ruijie Yin, Eric Christopher Brown, Brandon Hochahn Lee, Camilla Rodrigues, Sheila Nainan Myatra, Mohit Kharbanda, Prasad Rajhans, Yatin Mehta, Subhash Kumar Todi, Sushmita Basu, Suneeta Sahu, Shakti Bedanta Mishra, Rajesh Chawla, Pravin K. Nair, Rajalakshmi Arjun, Deepak Singla, Kavita Sandhu, Vijayanand Palaniswamy, Arpita Bhakta, Mohd-Basri Mat Nor, Tai Chian-Wern, Ider Bat-Erdene, Subhash P. Acharya, Aamer Ikram, Nellie Tumu, Lili Tao, Gustavo Andres Alvarez, Sandra Liliana Valderrama-Beltran, Luisa Fernanda Jiménez-Alvarez, Claudia Milena Henao-Rodas, Katherine Gomez, Lina Alejandra Aguilar-Moreno, Yuliana Andrea Cano-Medina, Maria Adelia Zuniga-Chavarria, Guadalupe Aguirre-Avalos, Alejandro Sassoe-Gonzalez, Mary Cruz Aleman-Bocanegra, Blanca Estela Hernandez-Chena, Maria Isabel Villegas-Mota, Daisy Aguilar-de-Moros, Alex Castañeda-Sabogal, Eduardo Alexandrino Medeiros, Lourdes Dueñas, Nilton Yhuri Carreazo, Estuardo Salgado, Safaa Abdulaziz-Alkhawaja, Hala Mounir Agha, Amani Ali El-Kholy, Mohammad Abdellatif Daboor, Ertugrul Guclu, Oguz Dursun, Iftihar Koksal, Merve Havan, Suna Secil Ozturk-Deniz, Dincer Yildizdas, Emel Okulu, Abeer Aly Omar, Ziad A. Memish, Jarosław Janc, Sona Hlinkova, Wieslawa Duszynska, George Horhat-Florin, Lul Raka, Michael M. Petrov, Zhilin Jin
-
- Journal:
- Infection Control & Hospital Epidemiology / Volume 45 / Issue 5 / May 2024
- Published online by Cambridge University Press:
- 04 January 2024, pp. 567-575
- Print publication:
- May 2024
-
- Article
- Export citation
-
Objective:
To identify urinary catheter (UC)–associated urinary tract infection (CAUTI) incidence and risk factors.
Design:A prospective cohort study.
Setting:The study was conducted across 623 ICUs of 224 hospitals in 114 cities in 37 African, Asian, Eastern European, Latin American, and Middle Eastern countries.
Participants:The study included 169,036 patients, hospitalized for 1,166,593 patient days.
Methods:Data collection took place from January 1, 2014, to February 12, 2022. We identified CAUTI rates per 1,000 UC days and UC device utilization (DU) ratios stratified by country, by ICU type, by facility ownership type, by World Bank country classification by income level, and by UC type. To estimate CAUTI risk factors, we analyzed 11 variables using multiple logistic regression.
Results:Participant patients acquired 2,010 CAUTIs. The pooled CAUTI rate was 2.83 per 1,000 UC days. The highest CAUTI rate was associated with the use of suprapubic catheters (3.93 CAUTIs per 1,000 UC days); with patients hospitalized in Eastern Europe (14.03) and in Asia (6.28); with patients hospitalized in trauma (7.97), neurologic (6.28), and neurosurgical ICUs (4.95); with patients hospitalized in lower–middle-income countries (3.05); and with patients in public hospitals (5.89).
The following variables were independently associated with CAUTI: Age (adjusted odds ratio [aOR], 1.01; P < .0001), female sex (aOR, 1.39; P < .0001), length of stay (LOS) before CAUTI-acquisition (aOR, 1.05; P < .0001), UC DU ratio (aOR, 1.09; P < .0001), public facilities (aOR, 2.24; P < .0001), and neurologic ICUs (aOR, 11.49; P < .0001).
Conclusions:CAUTI rates are higher in patients with suprapubic catheters, in middle-income countries, in public hospitals, in trauma and neurologic ICUs, and in Eastern European and Asian facilities.
Based on findings regarding risk factors for CAUTI, focus on reducing LOS and UC utilization is warranted, as well as implementing evidence-based CAUTI-prevention recommendations.
Crystallochemical characterization of the palygorskite and sepiolite from the Allou Kagne deposit, Senegal
- E. García-Romero, M. Suárez, J. Santarén, A. Alvarez
-
- Journal:
- Clays and Clay Minerals / Volume 55 / Issue 6 / December 2007
- Published online by Cambridge University Press:
- 01 January 2024, pp. 606-617
-
- Article
- Export citation
-
The Allou Kagne (Senegal) deposit consists of different proportions of palygorskite and sepiolite, and these are associated with small quantities of quartz and X-ray amorphous silica as impurities. No pure palygorskite or sepiolite has been recognized by X-ray diffraction. Textural and microtextural features indicate that fibrous clay minerals of the Allou Kagne deposit were formed by direct precipitation from solution. Crystal-chemistry data obtained by analytical/transmission electron microscopy (AEM/TEM) analyses of isolated fibers show that the chemical composition of the particles varies over a wide range, from a composition corresponding to palygorskite to a composition intermediate between that of sepiolite and palygorskite, but particles with a composition corresponding to sepiolite have not been found. Taking into account the results from selected area electron diffraction and AEM-TEM, fibers of pure palygorskite and sepiolite have been found but it cannot be confirmed that all of the particles analyzed correspond to pure palygorskite or pure sepiolite because both minerals can occur together at the crystallite scale. In addition, the presence of Mg-rich palygorskite and very Al-rich sepiolite can be deduced.
It is infrequent in nature that palygorskite and sepiolite appear together because the conditions for simultaneous formation of the two minerals are very restricted. The chemical composition of the solution controls the formation of the Allou Kagne sepiolite and palygorskite. The wide compositional variation appears as a consequence of temporary variations of the chemical composition of the solution.
Mental health research in South America: Psychiatrists and psychiatry trainees’ perceived resources and barriers
- Rodrigo Ramalho, Vanessa Chappe, Lisette Alvarez, Gianfranco C.A. Argomedo-Ramos, Guillermo Rivera Arroyo, Graciela L. Bonay, Javiera C. Libuy Mena, Miguel A. Cuellar Hoppe, Domenica N. Cevallos-Robalino, Jairo M. Gonzalez-Diaz
-
- Journal:
- Cambridge Prisms: Global Mental Health / Volume 10 / 2023
- Published online by Cambridge University Press:
- 02 October 2023, e66
-
- Article
-
- You have access Access
- Open access
- HTML
- Export citation
-
As mental health issues continue to rise in Latin America, the need for research in this field becomes increasingly pressing. This study aimed to explore the perceived barriers and resources for research and publications among psychiatrists and psychiatry trainees from nine Spanish-speaking countries in South America. Data was collected through an anonymous online survey and analyzed using descriptive methods and the SPSS Statistical package. In total, 214 responses were analyzed. Among the participating psychiatrists, 61.8% reported having led a research project and 74.7% of them reported having led an academic publication. As for the psychiatry trainees, 26% reported having conducted research and 41.5% reported having published or attempted to publish an academic paper. When available, having access to research training, protected research time and mentorship opportunities were significant resources for research. Further support is needed in terms of funding, training, protected research time and mentorship opportunities. However, despite their efforts to participate in the global mental health discussion, Latin American psychiatrists and psychiatry trainees remain largely underrepresented in the literature.
Proinflammatory activation profile in circulating monocytes in patients with a major depressive episode
- L. Grendas, R. Alvarez Casiani, A. Arena, M. Penna, F. Hunter, A. Olaviaga, C. Prokopez, V. Tifner, A. Armesto, A. Carrera Silva, A. Errasti, F. Daray
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S993-S994
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Mood Disorder (MD) affects more than 300 million people globally, and its etiology is unknown. In recently published data, MD has been correlated with inflammation and the immune system. Circulating monocytes have been proposed to play a role in the pathophysiology of depression.
ObjectivesTo determine if there is a specific activation profile of monocytes in patients with MD that differentiates them from healthy control (HC).
MethodsStudy Design: Case-control study matched by sex and age. The study was approved by IRB and carried out in three hospitals in Argentina.Participants between 18 and 55 years old from both genders, were evaluated by psychiatrists using the International Psychiatry Interview (MINI) to diagnose Mood Disorder (MD), and the Hamilton Depression Rating Scale (HADRS) to define active disease (AD), non-active disease (NAD) or healthy control (HC). The three monocyte subtypes were directly stained and analyzed in a drop of 100 uL of blood sample based on our validated monocyte cocktail including CD11b, HLA-DR, CD86, CD14 and CD16 expression by flow cytometry. To define normality Kolmogorov-Smirnov test was employed. A parametric T-test with Welch´s correction was employed for normal distribution and a non-parametric Mann Whitney test was used when comparing populations that do not pass the normality test.
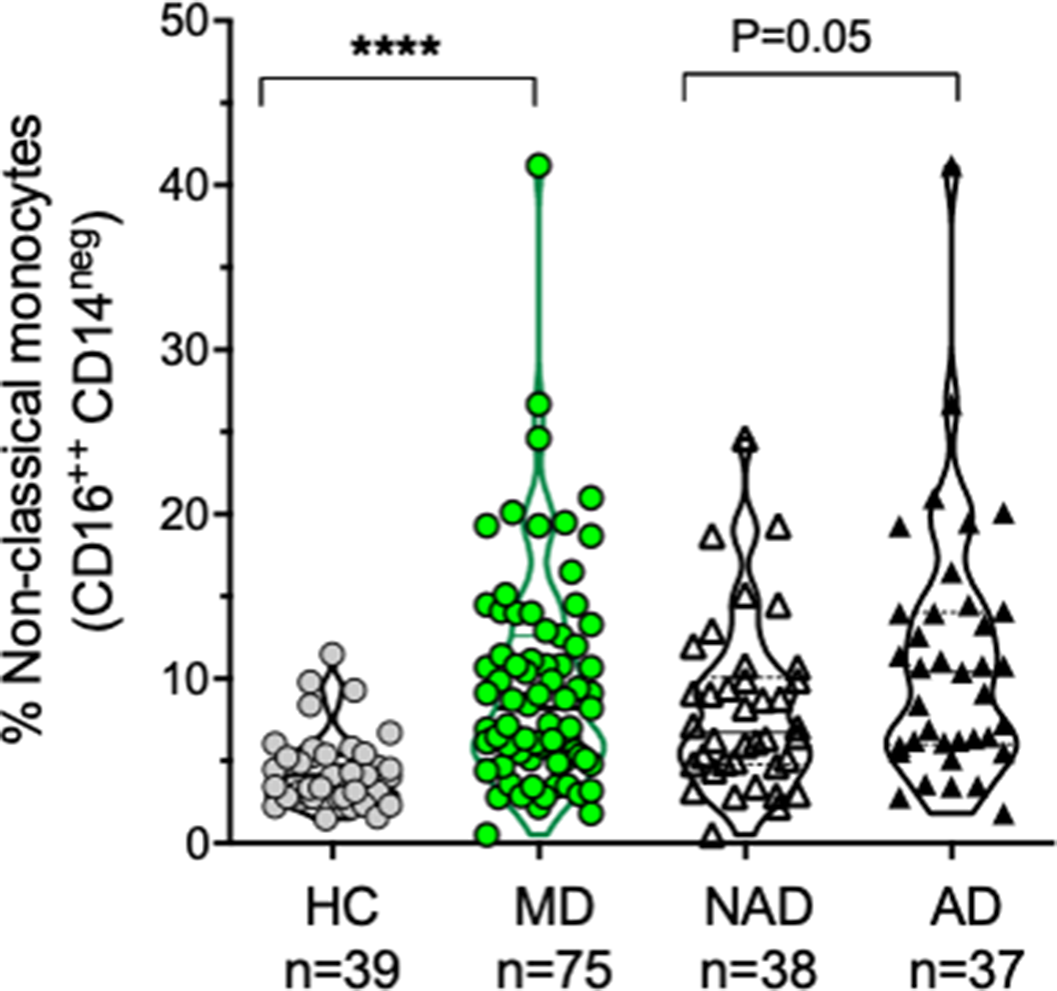
ResultsThe sample characteristics were shown in Table 1. Patients with AD (Hamilton >7) (n: 37), patients with NAD (Hamilton <7) (n: 38), and HC (n: 39) were recruited. The percentage of classical monocytes decreased in AD vs NAD (p=0.04), both AD, and NAD have significantly lower levels of classical monocytes than HC (****p<0.001) (Image 1). The percentage of intermediate monocytes is higher in AD vs NAD (p=0.05), both AD, and NAD have significantly higher levels of intermediate monocytes than HC (****p<0.001) (Image 2). The percentage of non-classical monocytes is higher in AD vs NAD (p=0.05), both AD, and NAD have significantly higher levels of non-classical monocytes than HC (****p<0.001) (Image 3).
Table 1. General characteristics of the sample
Active disease Non-active disease Healty control n 37 38 39 Age (SD) 42.95 (11.78) 42 (12.02) 40.67 (11.42) Women (%) 76.3 64.9 76.9 BD I 15.8 54.1 0.0 BD II 26.3 5.4 0.0 BD (non specified) 0.0 2.7 0.0 MDD 57.9 37.8 0.0 HAM-D 17 items mean (SD) 14.13 (4.89) 3.11 (2.35) 0.49 (0.85) Image:
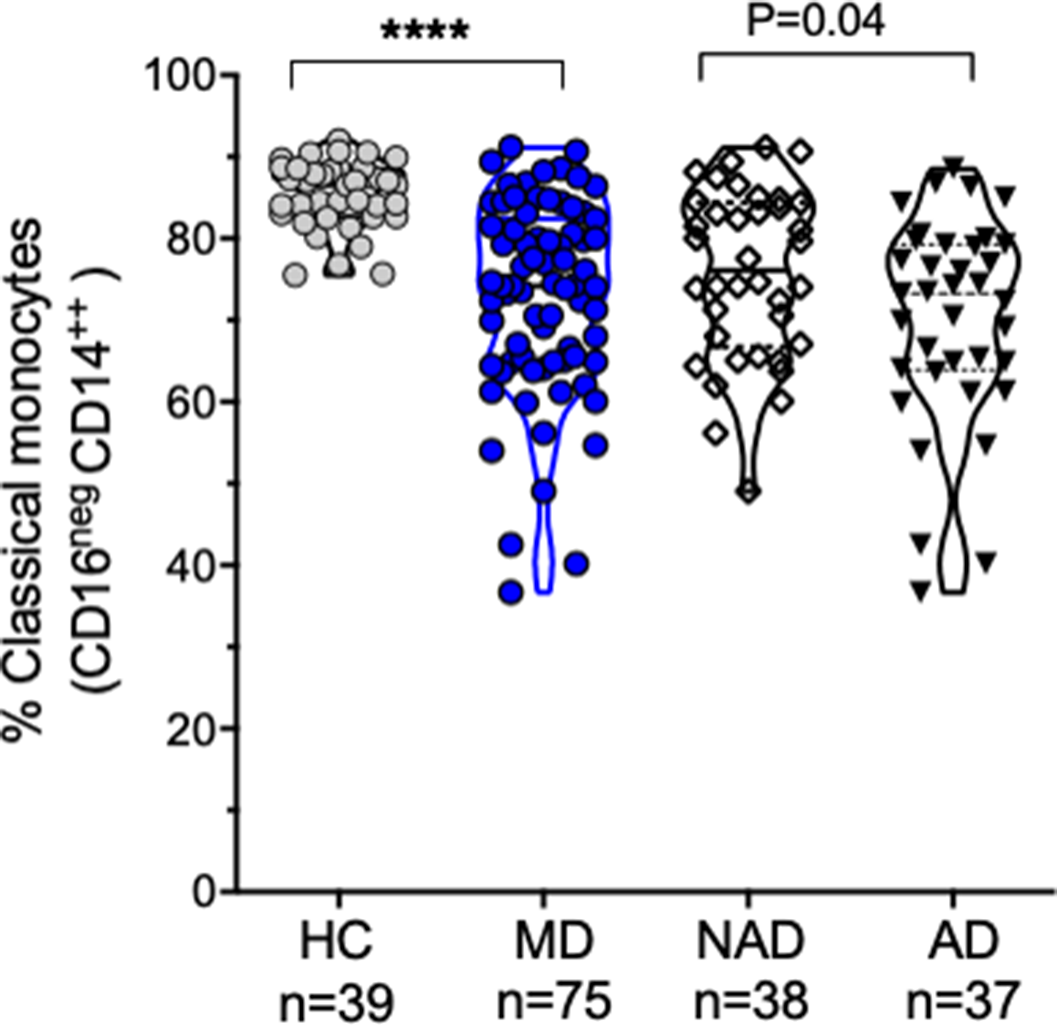
Image 2:
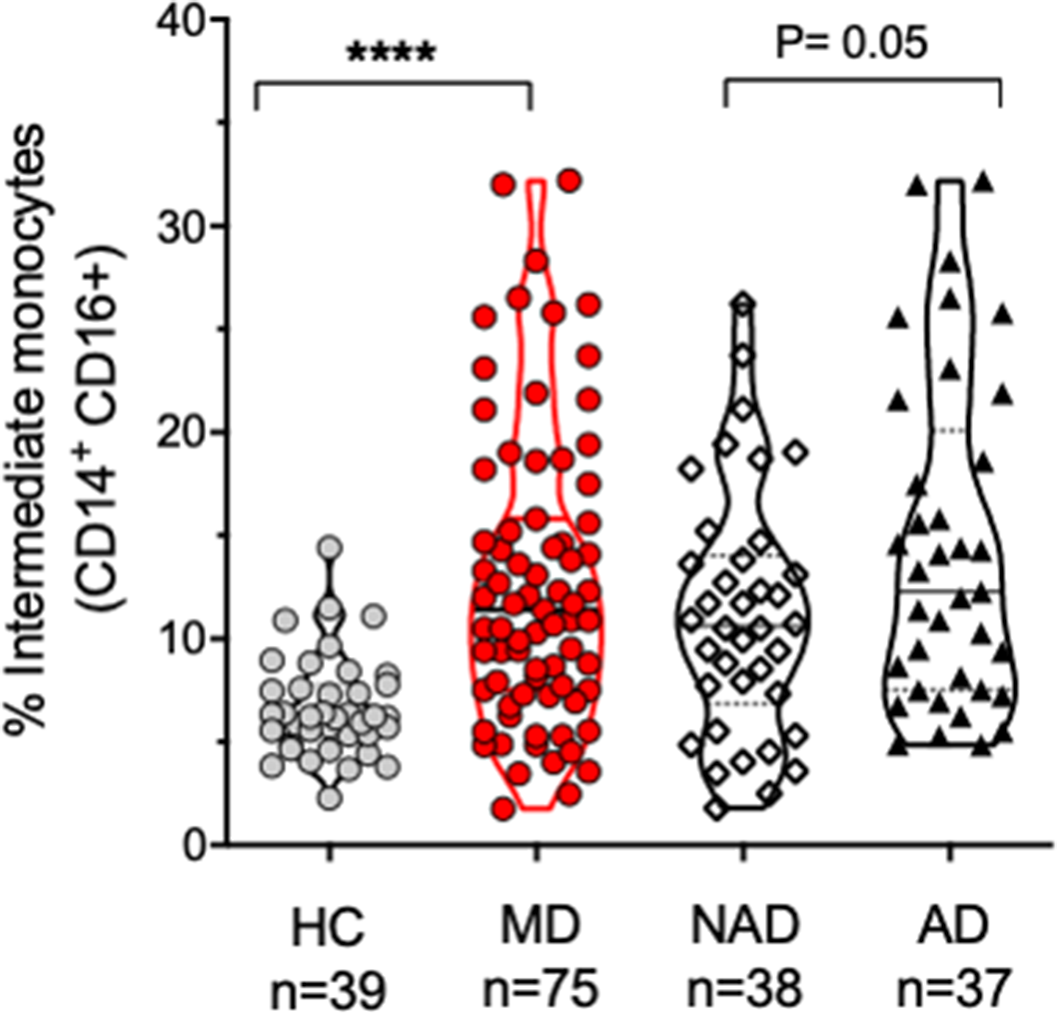
Image 3:
 Conclusions
ConclusionsWhile comparing percentages of three different monocyte subsets, clear differences in their distribution among the control and patient groups were appreciated. After comparing the subset frequencies between active patients (AD) and patients who were in remission (NAD), significant differences among the subsets were found although without reaching values of the HC, indicating that even patients in remission show an activated monocyte profile.
Disclosure of InterestNone Declared
Biomarkers and clinical predictors of long-term course in obsessivecompulsive disorder: A prospective cohort study
- S. López-Rodriguez, P. Alonso Ortega, C. Segalàs Cosi, E. Real Barrero, S. Bertolín Triquell, C. Soriano Mas, Á. Carracedo Alvarez, J. M. Menchón Magriña
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S231
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The purpose of the research project is to analyze the long-term evolution of obsessive-compulsive disorder (OCD) from of a study of a cohort of patients prospectively followed over a period ranging from 5 to 20 years, treated for according to therapeutic guidelines mediating serotonin reuptake inhibitors (IRS) and drug enhancers (antipsychotics) and cognitive behavioral therapy and evaluated in a standardized manner.
ObjectivesTo assess the long-term course of Obsessive-Compulsive Disorder (OCD) in a cohort of patients treated according to current clinical guidelines; to analyse possible prognostic factors associated with the long-term course of the disorder including clinical and sociodemographic variables, as well as genetic and neuroimaging biomarkers, and their interaction, and finally to study neuroanatomical and functional cerebral connectivity changes after 15 years of treatment in a subsample of patients.
MethodsProspective, descriptive, and observational study of a cohort of OCD patients, receiving treatment at the Department of Psychiatry of Hospital de Bellvitge since 1998, according to a standardized protocol. Follow-up period ranges from 5 (n=423), to 10 (n= 247) and 15 years (123). Baseline clinical and sociodemographic assessment, long-term evolution and information on treatments provided are available for the whole sample. Data on whole exome sequencing is available for 300 of the patients included in the cohort and baseline structural neuroimaging and cerebral functional connectivity has been analysed in 168 subjects. To expand the analysis of genetic biomarkers, we propose the study of de novo variants through exome analysis of 50 trios (patient and both parents) selected among those subjects that have reached 15 years of follow-up (25 trios with patients within the “long-term remission” group and 25 trios with patients with chronic OCD). De novo variants detected in the trio analysis will be replicated in the rest of the sample. A structural and resting state MRI will be obtained in a subsample of 100 patients recruited among those who have completed a minimum follow-up period of 15 years, to assess cerebral changes associated with the long-term course of the disorder.
Resultsin the current moment the recruitment period of the study has ended and all the data is being statistically analysed in order to provide solid results in a short period of time.
ConclusionsThe identification of those factors associated with an increased risk of chronic disease is an element essential to offer personalized treatment to our patients and improve their prognosis, emphasizing the intensive use of those therapeutic strategies for which we can predict a better response and modifying to the extent of, if possible, environmental factors or factors of access to treatment that contribute to perpetuate obsessive symptoms.
Disclosure of InterestNone Declared
The impact of the COVID-19 pandemic on health outcomes in delusional disorder: A systematic review
- E. Román, M. Natividad, M. V. Seeman, E. Izquierdo, E. Martínez, E. Rial, A. Alvarez, A. Guàrdia, J. A. Monreal, A. González-Rodríguez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S790
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The health impact of the COVID-19 pandemic has been widely recognized in both physical and mental health. Relatively little attention has been paid to patients with delusional disorder (DD).
ObjectivesOur goal was to synthesize the known mental and physical health consequences of the COVID-19 pandemic in patients diagnosed with DD.
MethodsA systematic review was carried out using the PubMed and Scopus database (2019-October 2022) following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) statement. Search terms: “delusional disorder” or “delusional disorder” AND “COVID-19 OR SARS-CoV2.” Inclusion criteria: 1)DD according to DSM/ICD, 2)languages: English, French, German and Spanish, 3)studies reporting health consequences of COVID-19 pandemic. From a total of 615 records, 6 were included: meta-analysis (n=1), cross-sectional studies (n=2), retrospective study (n=1), case reports (n=2).
ResultsA full third of patients with psychosis (including DD) presented with increased psychiatric symptom severity, reportedly activated by increased daily life stress. Suicidal behavior was reported in a previously undiagnosed DD patient in association with a worsening clinical picture. Perhaps surprisingly, admissions for DD in 2020 were lower than in 2019. The duration of hospitalization was, however, longer. There was a report of new onset DD with delusional material centred on COVID. There was also a report of COVID-19 symptoms being more severe in DD patients than in the larger community.
ConclusionsHealth emergencies affect the seriously mentally ill more than other community members. Awareness and outreach can help to maintain treatment adherence and minimize risk of psychotic exacerbation.
Disclosure of InterestNone Declared
TRANVIA: A program for continuum mental health assistance in transition period
- L. Pérez Gómez, A. González Álvarez, M. A. Reyes Cortina, E. Lanza Quintana, N. Álvarez Alvargonzález, C. Rodríguez Turiel, E. Lago Machado, J. J. Martínez Jambrina
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S728
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Transition between adolescence and adulthood represents the most important challenge for personal development and involves several transformations: physical, psychological and social. It is a complex age bracket, concurring the transition from youth psychiatric units to adult ones, with an increased risk for the appearance of mental disorders and risky behaviours. TRANVIA program, developed in Avilés, provides psychiatric assistance to patients between 15 and 25 years old, diagnosed with a severe psychiatric disorder or with an increased risk of having one.
ObjectivesOur objectives are: ensuring clinical continuity assistance, promoting communication among professionals and the empowerment of our patients to improve their functionality and quality of life.
MethodsDescriptive study including patients involved in TRANVIA program from November 2019 to November 2021.
ResultsDuring this two-years period there have been 44 referrals to the program, 11 of them were rejected for failure to comply with diagnostic criteria. In November 2021 there were 33 patients included in the TRANVIA program with an average age of 17 years old (range: 15-22). 70% of them were men and 30% women. All of them had psychiatric assistance from different sources: youth mental health units, neuropediatrics… About 75% of the patients were diagnosed with autistic spectrum disorder and approximately three-quarters of the sample needed pharmacological treatment. Risperidone was the most prescribed drug. We have also developed other assistance alternatives as home-based care, relaxation sessions, social worker interventions and coordination with schools.
ConclusionsTRANVIA program has allowed us to provide continual attention to vulnerable patients that shift from youth psychiatric units to adult ones. Patients that meet inclusion criteria were enrolled independently the type of assistance they have previously received. Accessibility and flexibility were our priority. During the described period there was only one dropout, three patients required psychiatric hospitalization and two others visited the emergency department. There have been no cases of completed suicide.
Disclosure of InterestNone Declared
An interesting clinical case. New therapies in Dissociative Identity Disorder.
- P. García Vázquez, E. Seijo Zazo, C. Vilellla Martin, A. Serrano García, C. M. Franch Pato, E. Martína Gil, C. Alvarez Vazquez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S970-S971
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Dissociative identity disorder (DID) also referred as multiple personality disorder is a chronic post-traumatic condition. It is characterized according to DSM-5 by “disruption of identity characterized by two or more distinct personality states”, with “marked discontinuity in sense of self… accompanied by related alterations in affect, behavior, consciousness, memory, perception, cognition, and/or sensory-motor functioning.”
ObjectivesHere, we present a case of a 33-year-old Caucasian female with no psychiatric history until 2 years ago, privately. The patient is admitted to the Psychiatry Service due to worsening. During admission, consultations are made to the Neurology Service and the Neurophysiology Service, who request an electroencephalogram, an MRI and a brain scan, resulting in normality.
After discharge, she returns home with her parents, and the crisis become more frequent and of longer duration. She acknowledges that during these periods she is dominated by her alternate personality, which she is unaware of until her family informs her. This personality is a demon, who verbally assaults and even physically threatens her surroundings, and can hardly be controlled by the prayers of her family.
MethodsDespite psychopharmacological treatment, as well as the cognitive-behavioral therapy carried out by the patient for more than two years, there was no improvement. Once she comes to the consultation, it is decided to carry out a therapy guided by the central Rogerian attitudes, originating a process of empathic resonance of the therapist, which influences the experience of the patient. Three main interventions are carried out, the awareness of the disease, the regulation of the intensity of this experience, to maintain the attention and the exploration of what guides the change. After carrying out this intervention, the patient is currently asymptomatic.
ResultsCurrently, there are not evidence-based treatment guidelines. The most common approach is individual psychodynamic psychotherapy according to practice-based guidelines initiated by the International Society for the Study of Trauma and Dissociation.
To handle the present case, we used a model with two pillars, the patient’s commitment and the investigation of microprocesses within a process of experiential exploration, in which the therapist is a facilitator of reflective attention and experimental awareness.
ConclusionsThe torpid evolution suffered by the patient, with little clinical improvement to the interventions carried out, and the absence of evidence on the treatment, led to a therapeutic approach focused on the empathic resonance process of the therapist, with good results.
Disclosure of InterestNone Declared
Parental Alienation Syndrome (PAS). Psychological and legal implications
- M. Arrieta Pey, S. Rubio Corgo, A. Álvarez Astorga, A. M. Delgado Campos, C. Díaz Gordillo, A. C. Castro Ibáñez, M. Á. Álvarez de Mon González
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S729-S730
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The first definition of PAS, enunciated by Richard Gardner in 1985, refers to a disorder originating in the context of legal conflicts related to child custody. Its main characteristic would be a smear campaign by the child towards a parent, in the absence of plausible arguments. In this context, the child would experience an oppositional and dichotomous feeling towards his or her parents. In recent years, the presence of PAS has become increasingly important, both in the legal and health fields, largely due to the controversy and debate surrounding its approval and recognition, and there is currently no consensus on the matter.
ObjectivesThe main objective of this work is to examine the current state of PAS in depth in the different fields in which it is emerging: the medical-scientific and legal spheres. The current controversies and debate, both scientific and legal, will be developed. Research will be carried out on the origin of the concept and its evolution, its symptomatic presentation, the neuropsychological consequences in minors, the role and legal value of expert reports, as well as the existing evaluation methods for the assessment of PAS.
MethodsAn extensive literature review was carried out on the subject in question, extracting information mainly from scientific articles, but also from legislative documents, manuals and books.
ResultsThere are currently no specific laws regulating PAS in European countries. According to Article 10.2 of the Spanish Constitution, norms related to fundamental rights shall be interpreted according to the Universal Declaration of Human Rights. As a direct consequence of the chronic psychological stresses experienced by children, adaptive disorders may appear, often characterised by symptoms of anxiety and depression. In addition, a multitude of neuropsychological consequences have been observed not only in the affected child, but also in the adult he or she will become.
ConclusionsCurrently, there is a fervent debate about the validity and recognition of PAS as a diagnostic entity, spanning different disciplines, ranging from health to social and legal. In Europe, professionals in the scientific field have not reached an agreement regarding the approval of PAS. On the one hand, there are those for whom PAS is a verified phenomenon; on the other hand, there are those who flatly reject the existence of this phenomenon. The latter consider PAS an unscientific construct, referring to it as “court syndrome” or “patriarchal alienation syndrome”.
Disclosure of InterestNone Declared
Stigma and self-stigma in patients with delusional disorder: a systematic review.
- A. González- Rodríguez, A. Alvarez, E. Román, A. Guàrdia, M. Natividad, M. Alberto Marcus, E. Calvo, J. Labad, J. A. Monreal
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1044
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The association between insight, stigma and self-concept has been considered as a potential predictor of poor clinical outcomes and global functioning in psychosis. In patients with delusional disorder (DD), the effects of stigma and self-stigma have been poorly explored.
ObjectivesOur main goal was to systematically review studies addressing stigma and self-stigma in DD to assess whether these phenomena have an impact on clinical symptoms.
MethodsA systematic review was conducted through PubMed and Google Scholar databases from inception to 2022 (PRISMA guidelines). Search terms: (Stigma OR self-stigma) AND (“delusional disorder” OR psychosis OR paranoia). Studies were considered eligible if they included patients with DD.
ResultsA total of 875 records were retrieved, from which 18 were included.
Stigma: (1) Stigma is associated with poor quality of life, poor adherence to medications and acceptation of diagnosis. (2) Support at workplaces would improve stigma and discrimination in DD. (3) Poor interpersonal competence may increase stigma experience in DD.
Self-stigma: (1) Women show higher level of self-stigma than men. (2) Higher rates of psychiatric hospitalizations and higher severity of symptoms associated with greater degree of self-stigma. (3) Suicidal ideation was associated with negative self-schema but not self-stigma, particularly in patients with persecutory delusions. (4) Self-stigmatization negatively associated with quality of life. (5) Depressive symptoms associated with higher levels of self-stigma. (6) Promotion interventions should address self-stigma content.
ConclusionsFurther longitudinal studies are needed to test the influence of stigma and self-stigma on adherence to follow-up and specific interventions to improve them.
Disclosure of InterestNone Declared
“Unspecified organic personality and behavioral disorder due to brain damage from HHV-6 encephalitis in child. case report and literature review”
- A. Oliva Lozano, M. A. Morillas Romerosa, P. Herrero Ortega, J. Garde Gonzalez, B. Orgaz Álvarez, J. Curto Ramos, M. Alcamí Pertejo
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S143-S144
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We present a case of a 15 year-old boy diagnosed with Unspecified Personality and Beheavioral Disorder Due to Brain Damage from a Human Herpes Virus-6 Encephalitis.
ObjectivesTo describe a case of an Unspecified Organic Personality and Behavioral Disorder secondary to brain damage from Human Herpes Virus-6 (HHV-6) Encephalitis in an 11 year-old childand to review recent literature, in order to improve clinical practice.
MethodsClinical case report and brief review of literature. A bibliographic research was made in the database PubMed, using the terms “Viral Encephalitis” AND “Neuropsychiatric symptoms”; “Viral Encephalitis” AND “Behavioral Disorder”; “Long-Term Neurological Morbidity” AND “Viral Encephalitis”.
Results15 year-old boy diagnosed with Unspecified Personality and Beheavioral Disorder Due to Brain Damage from a Human Herpes Virus-6 Encephalitis, secondary to immunosupression in the context of haematopoietic progenitor transplantation (HPT) at 11 years old. MRI showed supratentorial ventriculomegaly, atrophic changes in encephalon and right hippocampus with subcortical retraction secondary to previous encephalitis. Clinically, main changes appeared in behavior, presenting a serious frontal syndrome with high disinhibition, what implied severe social and academic difficulties. During the outpatient follow-up, the behavioural disorder is being pharmacologically treated with Risperidone 1,5mg per day with a partially favorable evolution. The patient presented intolerance to olanzapine, with an episode of low level of conciuosness after taking it.
Bibliographic research results indicate that the gold standard treatment for behavioral disturbances are antipsychotics. Risperdidone is proven save for treatment in children. Results point out also the importance of an early multidisciplinar intervention, involving family training, rehabilitation resources and curricular adaptations.
Image:
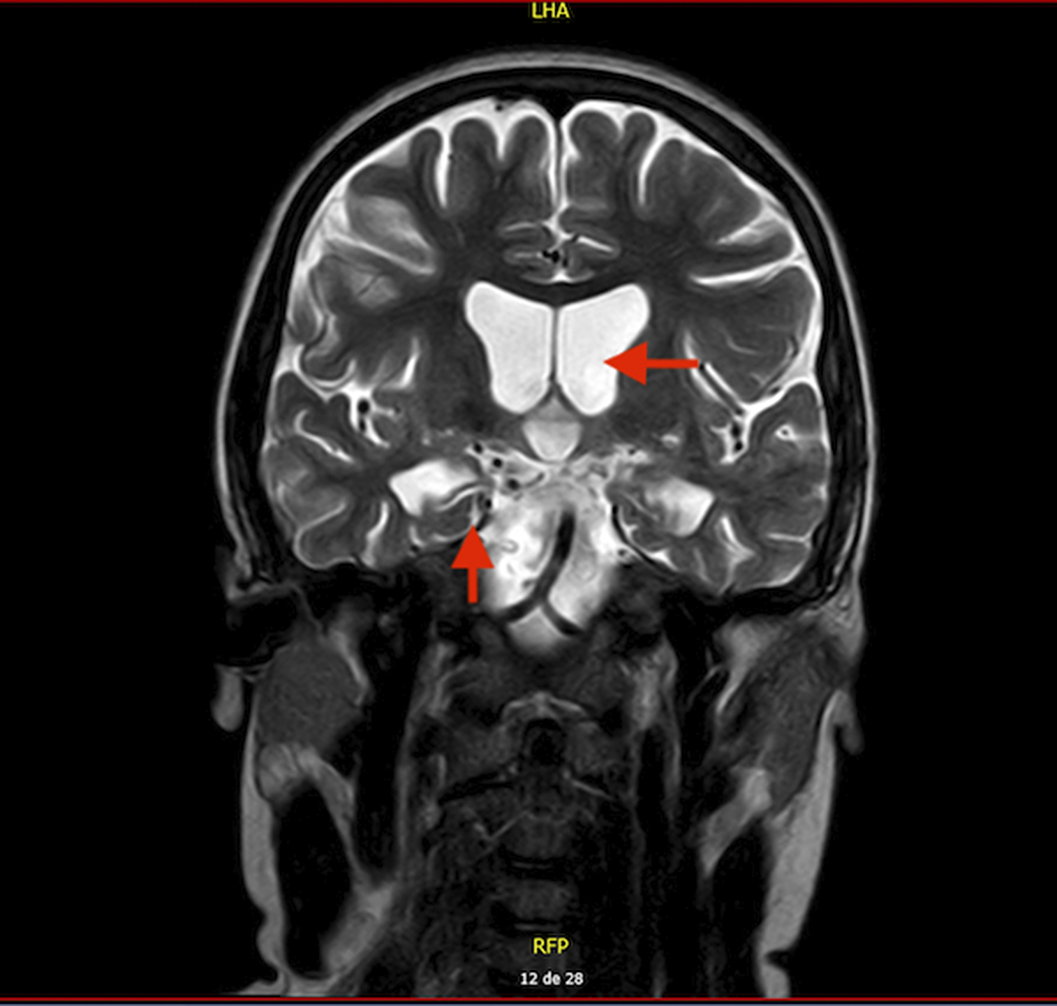
Image 2:
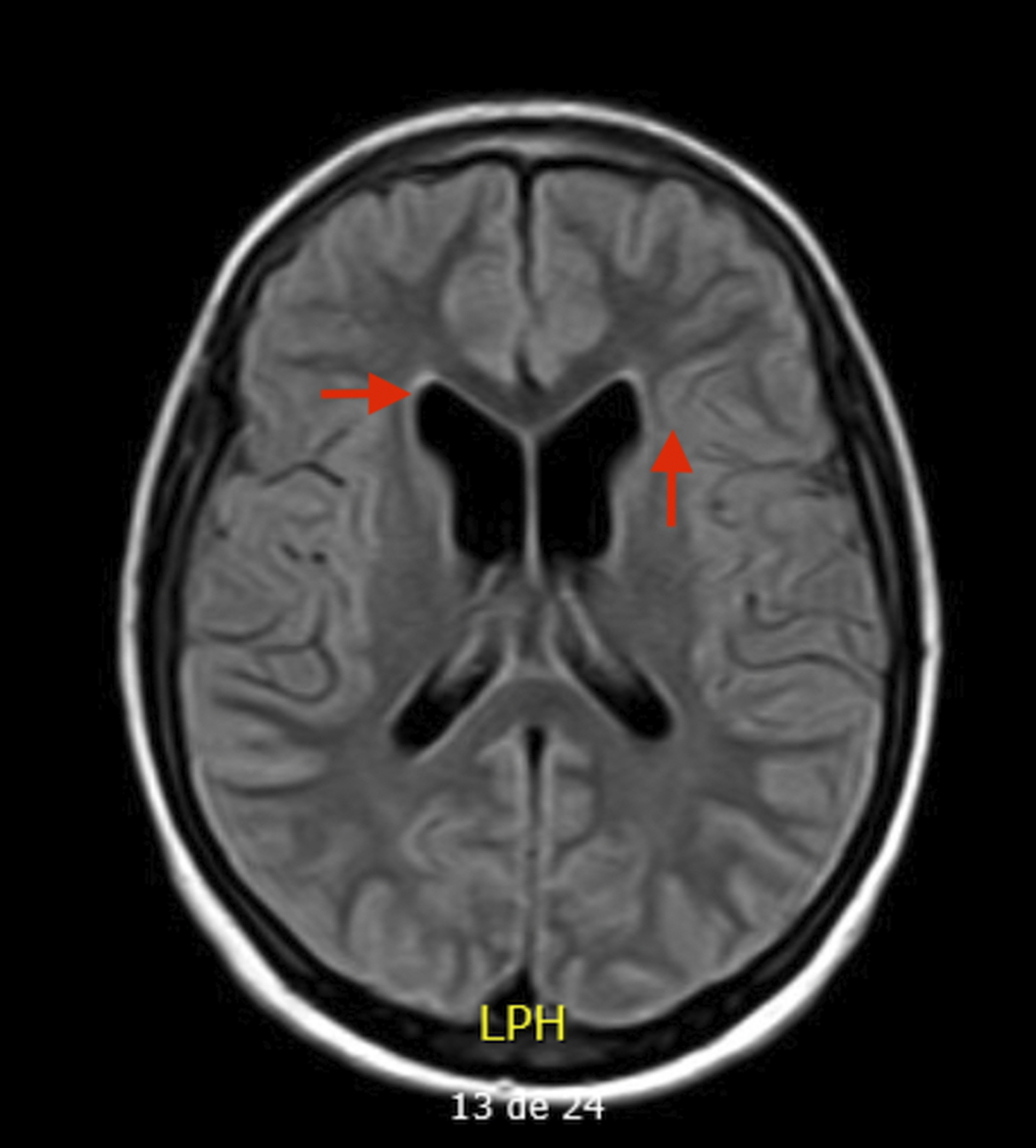 Conclusions
ConclusionsViral encephalitis may have serious neuropsychiatric consequences, especially during childhood while the brain development is not finished. When the neurological damage affects the frontal lobes of the brain, behavioural and personality disturbances are expected and an early multidisciplinar intervention should be considered. Antypsichotics are the gold standard pharmacological treatment for behavioural disturbances. During the scholar period, special curricular adaptations should be done in order to reduce study-related stress.
Disclosure of InterestNone Declared
Alcohol use in adult patients with autism spectrum disorder (ASD). Case report
- P. Del Sol Calderon, A. Izquierdo de la Puente, A. Alvarez Astorga, M. García Moreno, R. Fernandez Fernandez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S762
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Patients with autism spectrum disorder are characterized by high anxiety when facing social situations and dealing with interpersonal relationships on a daily basis. Although initially because of their rigid personality with the norm, and their tendency to social distancing, we do not have in mind this pathology as the most likely to develop a substance use disorder. However, it is observed in the literature a remarkable percentage of patients who resort to consumption, mainly alcohol, as an anxiolytic to be able to interact in society.
ObjectivesTo show the case of a 19-year-old adult with a diagnosis of ASD who resorts to alcohol consumption in her daily life as a strategy to manage anxiety in social situations.
MethodsCase report and literatura review
ResultsThis is a 19-year-old woman with a recent diagnosis of ASD. She is studying biotechnology and lives with her parents and 3 siblings. The patient reports difficulty in social relationships since early childhood, with experiences of school bullying. She expresses desire to relate with others, although she does it in an inadequate way, with difficulty in detecting nonverbal language, irony and anger when she does not understand a joke. The patient confesses that since she was 16 years old she has consumed alcohol to mitigate the anxiety caused by facing a group of people. She says that she feels that it relaxes her and facilitates interaction, making it more fluid and less tense. However, she recognizes that initially she used to drink 1 or 2 beers, but now she needs to drink up to 2 glasses of gin, recognizing this as something problematic.
ConclusionsThe literature shows how patients with ASD can also present substance use disorder. It has been shown that about 10% of these patients have an abusive use of alcohol. Other samples show wider ranges (7-71%) of prevalence of alcohol consumption in patients with autism. In relation to cannabis, it is seen that around 3% of these patients consume it. These patients seek its anxiolytic effect and to reduce mental health symptoms. In addition, the purchase of alcohol does not involve high social interaction to obtain it, since it is a substance that can be purchased legally. It is important to explore alcohol consumption in consultation with patients with ASD to help them develop more functional anxiety management strategies.
ReferencePrevalence of psychiatric disorders in adults with autism spectrum disorder: A systematic review and meta-analysis. Lugo-Marín.J et al. 2019. Research in Autism Spectrum Disorders Volume 59, March 2019, Pages 22-33
Disclosure of InterestNone Declared
Use of paliperidone palmitate half-yearly release in patients diagnosed with psychotic disorder: profile and satisfaction of use
- P. Andres-Olivera, A. Alvarez, M. D. L. A. Garzon, R. Gonzalez, C. Roncero, P. Jesús
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S638
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
The lack of insight can be present among patients with a diagnosis of schizophrenia, which often results in lack of adherence to pharmacological treatments1 and, subsequently, in treatment discontinuation and relapses2. This vicious pattern leads to further clinical deterioration, impaired functioning, and reduced quality of life 3. There is a plethora of evidence supporting the fact that long-acting injectable and depot antipsychotics can increase adherence to treatment, reduce the risk of discontinuation and hospital admissions4. It is also known that low fluctuations between peaks and lows in plasma drug levels could be related to a better tolerability profiles5. A new paliperidone palmitate prolonged release formulation, which is administered twice annually, has been approved as maintenance treatment for patients with schizophrenia who are already stable on the monthly or quarterly prolonged release paliperidone palmitate6.
ObjectivesWe aimed to evaluate the transition of monthly and quarterly paliperidone palmitate to the new six-monthly formulation and patients’ satisfaction with it in a real-world clinical setting.
MethodsWe collected a basic epidemiologic questionnaire, responses to a query about local pain after administration, and the Drugs Attitude Inventory (DAI).
ResultsA total of 21 patients from an outpatient clinic for severe mental disorders with a long evolution of their disease in Salamanca, Spain, were included. All of them had a DSM5-TR diagnosis of Schizophrenia. Sixteen were male and 5 female. The mean age was 42.6 years. 14 were receiving quartlery paliperidone palmitate (10 with high doses (525 mg) and 4 with moderate doses (350 mg)) and 7 were on monthly injections (6 with high doses (150 mg) and 1 with a moderate dose (100 mg)). Those receiving moderate doses of quarterly or monthly paliperidone palmitate were administered 700 mg of six-monthly paliperidone palmitate; 1000 mg were injected to those with higher doses. The mean score on the DAI scale was 8. Only one patient reported an increase in local pain after the injection, and another reported dissatisfaction with the administration in the gluteus instead of the deltoid muscle. The first administration of the new formulation in our site was on June 26th; to date none of these patients have required hospital admission due to relapse.
ConclusionsSix-monthly prolonged release paliperidone palmitate seems to be an effective maintenance treatment for schizophrenia. In addition, this new formulation is well received and tolerated by patients previously on monthly or quarterly formulations of the same drug.
Disclosure of InterestNone Declared
Chronic disease (CD) during transition from child to adult.Psychopathological consequences and coping strategies
- S. Rubio Corgo, M. Arrieta Pey, A. M. Matas Ochoa, M. I. Duran Cristobal, E. Perez Vicente, A. Delgado Campos, C. Diaz Gordillo, A. C. Castro Ibañez, A. Alvarez Astorga, P. Alcindor Huelva
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S745
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
CD is characterized by at least three features: its duration is prolonged, it does not resolve spontaneously and it is rarely completely cured. Approximately 10-15% of young people have CD. Adolescents with CD often have emotional and behavioral problems.
ObjectivesTo assess risk factors, derived psychiatric pathologies and coping strategies for a CD diagnosis in adolescence.
MethodsAn extensive literature review was carried out on the subject in question, extracting information mainly from scientific articles, manuals and books.
ResultsThe main risk factors are those related with the CD in question, physical sequelae, the need for long-term hospital admissions or the use of drugs whose side effects include affective or behavioral symptoms; those related to the personality traits of the affected child or adolescent. In addition, as far as the family is concerned, the presence of a low level of education, lack of support or communication, as well as the presence of psychiatric disorders or serious medical conditions in parents. Among the most frequent psychiatric disorders associated with CD are affective and anxiety disorders, adaptive disorders, somatoform disorders, eating disorders and behavioral disorders. Whatever the CD is, it generates high levels of stress and uncertainty in the patient and family, which must be dealt together from a flexible perspective, allowing child or adolescent to adapt to the changes, reorganize and facing them with adaptive patterns of behavior. For this, it will be essential to have adequate social and family support with relational style based on communication, trust and acceptance.
ConclusionsIn general, both adolescents with CD and their families have an adequate capacity to adapt to the repercussions and effects derived from the disease. Nevertheless, in case of possible emotional difficulties that may appear, a comprehensive and individualized approach to these adolescents and their families is necessary to provide them resources and coping strategies in different areas and contexts in which the disease debuts.The comprehensive therapeutic approach will consist of interventions at the individual and family level. Among the main objectives of these interventions are to achieve acceptance and adaptation to CD provinding adequate psychosocial support to enable them to cope with CD in the best possible way and to detect and address the emotional implications, even coexisting psychopathology.
Disclosure of InterestNone Declared
Extrapyramidal syndrome in psychotic depression: a case report.
- C. Álvarez, A. M. Gómez Martín
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S1049-S1050
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Psychotic depression is a subtype of major depression, with worst prognosis but underdiagnosed and undertreated. We introduce the case of a 75-year-old patient who is attended in the hospital presenting sorrow and behavioral disturbances. He also had delusions of ruin and surveillance through his phone, adding amnesia, dizziness, constipation, tremor and bradykinesia. He had suffered a limited depressive episode regarding his wife’s death.
ObjectivesTo highlight the importance of a correct differential diagnosis in psychotic depression to prescribe an adequate treatment that provides a better outcome for the patient.
MethodsA narrative search of the available literature on the subject through the presentation of a case.
ResultsThe presumptive diagnosis is Parkinson vs psychotic depression. After some weeks of treatment with venlafaxine and olanzapine, the absence of improvement and fluctuating symptoms orientates towards Parkinson. This is later excluded due to a normal DATSCAN. Therefore, the diagnosis of psychotic depression is made, explaining parkinsonism as secondary to psychotropics. Olanzapine and venlafaxine are retired, introducing clozapine because of its lower incidence of extrapyramidal symptoms. After two weeks, the symptoms disappear, recovering the patient his basal functionality.
ConclusionsDepression with psychotic symptoms can take several weeks to respond to treatment, requiring a proper organic screening. In our case, the slow response to treatment made the organic etiology as one of the main differential diagnoses, specifically Parkinson disease. It ruled out because of the absence of findings in the DATSCAN and the resolution of the extrapyramidal symptoms with the change of treatment.
Disclosure of InterestNone Declared
The use of long-acting injectable antipsychotics in an acute psychiatric unit
- G. Ortega-Hernández, N. Ramiro, F. Palma-Álvarez, Ó. Soto-Angona, M. F. Mantilla, J. Duque, I. Gonzalo, F. Collazos
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, pp. S182-S183
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Long-acting injectable antipsychotic (LAI) are an important and arguably under-utilized therapeutic option, particularly where medication adherence is a priority (Pilon et al. Clin Ther 2017; 39 1972-1985).
In recent years, meta-analytic reviews of depot medications concluded that this route of administration produced clinical advantages in terms of overall outcome, with lower probability of relapse, readmissions, shorter hospital admission time, mortality, and thus better long- term prognosis over other oral antipsychotics (Leucht et al. Schizophr Res 2011;127 83-92). Depot treatment is associated with lower overall medical expenditure (Taipal et al. Schizophr Bull 2018;17 1381- 1387).
ObjectivesTo describe the evolution of people diagnosed with a psychotic disorder 6 months before and after the introduction of long-acting injectable antipsychotic (LAI) in the acute psychiatric unit of San Rafael Hospital (Spain) from January 1, 2018 to December 31, 2018.
MethodsRetrospective and prospective naturalistic study. Patients with a diagnosis of psychotic disorder who were admitted to the acute psychiatric unit in 2018 and who were introduced to LAI (paliperidone palmitate, aripiprazole, olanzapine pamoate or risperidone), are selected. Sociodemographic variables (sex, age, ethnicity, migratory status, marital status, occupation, cohabitation) and clinical variables (main and secondary diagnosis, comorbidity with drug use and history of poor adherence) are described. The number of emergency visits and hospital admissions before and after the introduction of LAI antipsychotic treatment is compared.
ResultsThe sample was composed of 99 subjects. The mean age was 42.46 years (SD 13.439) and 67.7% were men. The socio-demographic profile was: european caucasian ethnicity (73.7%), non- migrant status (69.7%), single (67.7%), inactive (43.4%) and residing in the home of relatives (50.5%). 53.5% have a diagnosis of schizophrenia, followed by schizoaffective disorder (24.2%). 45.5% are diagnosed with any drug use disorder, the most frequent being cannabis (30.3%). 76.8% have a history of discontinuing oral treatment. There was a statistically significant decrease (p<0.0001) in number of emergency visits and hospital admissions after the introduction of LAI antipsychotic.
In the general linear multivariate before-after model, there were significant differences (p=0.002) in the number of admissions after long-term IM antipsychotic treatment. As for the comparison of the effects between the different LAIs, there are differences between them (p< 0.0001). Post-hoc analysis (Bonferroni) only showed differential significance for treatment with Paliperidone Palmitate (p<0.0001).
ConclusionsThe use of LAI antipsychotic can reduce the number of emergency room visits and hospital admissions, in line with literature.
Disclosure of InterestNone Declared
Changes in the characteristics of Suicide Attempts during COVID-19 pandemic
- J. Curto Ramos, N. Kishanchandani Chandiramani, M. Torrijos, J. Andreo-Jover, B. Orgaz-Alvarez, M. Velasco, D. García Martínez, G. Juárez, S. Cebolla, P. Aguirre, B. Rodríguez Vega
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S405
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Different studies indicate high prevalence’s of suicidal behaviour, anxiety, depression, insomnia, and PTSD associated with the COVID-19 pandemic. There is currently not enough scientific evidence available to analyze the impact that the COVID-19 pandemic has had on the rate of suicide attempts and their characteristics.
ObjectivesTo analyze and compare the characteristics of suicidal behavior (in terms of method, severity, medical damage produced and need for hospitalization) of patients attended during the COVID-19 pandemic compared to previous years.
MethodsA retrospective study was performed based on a standardized data collection of patients attending the University Hospital La Paz between April 2018 and November 2021. 581 patients who attempted suicide at least once were included in this study. We compared the severity using the Beck Suicide Intent Scale. Chi-square ant Student’s t were used to compare clinical characteristics such as medical damage, method of suicide attempt and indication for admission after the attempt, between suicide attempts during the COVID-19 pandemic and previous years.
ResultsOur results suggest that during the COVID-19 pandemic suicide attempts caused more medical damage (p<0.001), had higher severity (p<0.000), and required more admission in Intensive Care Units, General Internal Medicine and Psychiatry compared with pre-Covid years (p<0.000).
ConclusionsThis is the first study in Spain analysing the changes in characteristics of suicide attempts during the COVID-19 pandemic. This has important implications for reducing suicide rates, preventing future attempts, and enabling us to design specific treatments of Suicidal Behaviour.
Disclosure of InterestNone Declared
Psychosomatics and mentalization
- A. M. Delgado Campos, P. Alcindor Huelva, A. Alvarez Astorga, S. Rubio Corgo, E. Pérez Vicente, M. Arrieta Pey, C. Diaz Gordillo, P. Del Sol Calderón, A. C. Martín Martín
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1024
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
We have investigated the relationship between the Psychosomatic Classification method (Marty) and the Rorschach Test, with respect to the diagnosis of psychosomatic disorders, within the framework of the degree of mentalization measured by both.
ObjectivesA) To verify statistical coincidence with respect to the degree of mentalization (risk of generating psychosomatic disorders in a subject) between the Rorschach Test and the diagnostic technique Psychosomatic Classification, by P. Marty. B) To test the hypothesis: Patients diagnosed with infertility, whose degree of mentalization is good, will have a greater probability of achieving a successful pregnancy throught Assisted Reproduction Techniques.
MethodsTwo evaluation tools were used: a) Psychosomatic Classification based on the criteria established by this diagnostic method; b) The Rorschach test (based on the evaluation of 29 indicators, selected according to their greater relevance in the generation of somatic symptoms).
A sample of 120 patients (women) diagnosed infertility at the Assisted Reproduction Unit (U.R.A.) at Hospital Universitario 12 de Octubre in Madrid was recruited. The method of ‘statistical correlation of coincidence’ between the results of the two diagnostic instruments used was used. Once both tests had been assessed by the “inter-judge” method and the quantitative values of the selected items had been weighted, the KAPPA statistical method was applied to establish the “correlation of coincidence” between the results of the two assessment instruments.
ResultsConsidering that the KAPPA method takes values between “0" and ”1" and that between 0.6 and 0.8 the agreement or coincidence is considered good, and above 0.8 very good, the result applied to the hypothesis is 0’76 (’good’).
ConclusionsA) Using the Rorschach Test and P. Marty’s Psychosomatic Classification in a complementary manner, these two instruments together provide high reliability, with respect to the degree of mentalization (a subject’s risk of suffering psychosomatic disorders). B) The degree of mentalization has a significant impact on the success or failure in the application of Assisted Reproduction Techniques in infertile women.
Disclosure of InterestNone Declared








